Melasma 101: Everything You Need to Know
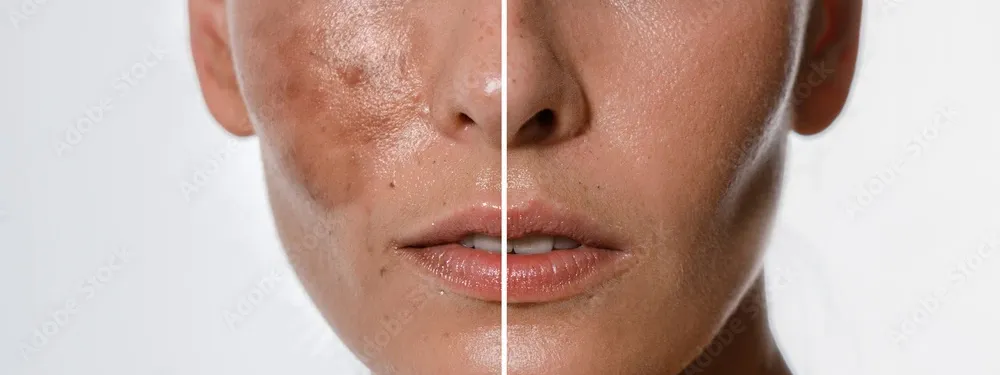

Melasma affects millions of people worldwide, yet many struggle to identify this common skin condition. Those brown or grayish patches that appear on your face might seem mysterious, but understanding what causes them and how to spot them early can make all the difference in your skincare journey. Whether you're dealing with pregnancy-related changes or noticing new discoloration, learning to recognize melasma helps you take the right steps toward clearer, more even-toned skin.
Melasma is a chronic skin condition that causes brown or grayish patches to appear on the face. Often called the "mask of pregnancy," this condition affects about 90% of women, though men can develop it too. The patches typically appear symmetrically on both sides of the face, creating a distinctive pattern that sets melasma apart from other types of skin discoloration. Unlike general hyperpigmentation that might result from acne scars or sun damage, melasma has specific characteristics. The patches are usually flat, smooth to the touch, and develop gradually over time. They don't itch or hurt, but they can significantly impact how you feel about your appearance. The condition is closely linked to hormonal changes, which explains why it's so common during pregnancy and among women taking birth control pills.
Learning how to identify melasma starts with understanding its unique visual characteristics. Unlike random dark spots, melasma follows specific patterns that make it recognizable once you know what to look for. The key is paying attention to the shape, location, and color of the patches.
Melasma patches have several telling features that help distinguish them from other skin conditions. They appear symmetrically on both sides of your face, creating a mirror-like pattern. The patches are completely flat with no raised texture, and they develop slowly over weeks or months rather than appearing suddenly.
The most common areas for melasma on face include the cheeks, bridge of the nose, and forehead. You might also notice patches on your upper lip area or along your jawline. The center of your face tends to be most affected, which is why dermatologists often refer to the "centrofacial pattern" when describing melasma.
The color of melasma patches varies depending on your natural skin tone. Fair-skinned individuals typically see light brown to tan patches, while those with medium skin tones notice grayish-brown discoloration. People with darker skin often develop bluish-gray patches that can be more challenging to treat.
Dermatologists classify melasma into different types of melasma based on where the patches appear on your face. Understanding these patterns helps both you and your healthcare provider identify the condition more accurately and choose the most effective treatment approach. The centrofacial pattern is the most common type, affecting the center of your face including your forehead, cheeks, nose, and upper lip. The malar pattern focuses primarily on your cheeks and nose area. The mandibular pattern appears along your jawline and is less common than the other two types.
This pattern covers the central area of your face in a butterfly-like distribution. It's the most recognizable form of melasma and often the most noticeable.
The malar pattern affects your cheekbones and the sides of your nose. This type might be mistaken for sun damage at first glance.
Less common than other types, this pattern appears along your jawline and can extend down toward your neck area.
Understanding melasma causes helps you make informed decisions about prevention and treatment. The condition results from a combination of factors, with hormones and sun exposure being the primary triggers. Your genetics also play a significant role in determining whether you'll develop melasma.
Hormonal changes are the biggest trigger for melasma development. Pregnancy hormones, particularly estrogen and progesterone, stimulate melanin production in susceptible individuals. Birth control pills and hormone replacement therapy can have similar effects. Even thyroid dysfunction can contribute to melasma development.
Sun exposure is the second major cause of melasma. UV radiation triggers melanin production, but interestingly, visible light and heat can also worsen the condition. This is why melasma often gets worse in summer months, even with sunscreen use.
Certain medications can increase your risk of developing melasma. Some cosmetic products, particularly those that irritate your skin, might trigger the condition. Stress and poor sleep can also contribute to hormonal imbalances that worsen melasma.
While you might suspect melasma based on visual signs, professional hyperpigmentation diagnosis ensures you get the right treatment. Dermatologists use several tools and techniques to confirm melasma and rule out other conditions that might look similar. The diagnostic process typically starts with a visual examination of your skin. Your dermatologist will look at the pattern, color, and distribution of the patches. They'll also ask about your medical history, including pregnancy, medication use, and sun exposure habits.
Dermatologists examine your skin under normal lighting and look for the characteristic symmetrical pattern of melasma. They'll note the color, size, and exact location of each patch.
A Wood's lamp uses ultraviolet light to make certain skin conditions more visible. Under this special light, melasma patches often become more pronounced, helping confirm the diagnosis.
This technique uses a special magnifying device to examine your skin more closely. It helps distinguish melasma from other types of pigmentation disorders.
Melasma treatment requires patience and often a combination of approaches. The good news is that several effective options exist, from gentle topical treatments to professional procedures. The key is finding the right approach for your skin type and lifestyle. Treatment success depends on several factors, including how long you've had melasma, its severity, and your commitment to sun protection. Most people see improvement within three to six months of consistent treatment, though complete clearing can take longer.
Topical treatments form the foundation of most melasma treatment plans. Hydroquinone remains the gold standard, often combined with tretinoin and mild corticosteroids. Vitamin C serums and kojic acid offer gentler alternatives for sensitive skin.
Chemical peels can help accelerate the removal of pigmented skin cells. Certain laser treatments target melasma, though they require careful selection based on your skin type. Microneedling combined with topical treatments shows promising results for some people.
The most effective melasma treatment often combines multiple approaches. Your dermatologist might recommend a topical treatment along with professional procedures and strict sun protection.
Melasma prevention focuses on avoiding known triggers and protecting your skin from further damage. Since melasma tends to recur, prevention becomes an ongoing part of your skincare routine rather than a one-time effort. Sun protection is absolutely essential for preventing melasma and keeping existing patches from getting darker. This means daily sunscreen use, protective clothing, and seeking shade during peak sun hours.
Use broad-spectrum SPF 30 or higher every day, even when it's cloudy. Physical sunscreens with zinc oxide or titanium dioxide often work better for melasma-prone skin. Don't forget protective clothing, wide-brimmed hats, and sunglasses.
If you're prone to melasma, discuss birth control options with your healthcare provider. During pregnancy, focus on gentle skincare and diligent sun protection since most treatments aren't safe for expecting mothers.
Gentle skincare routines help prevent irritation that might trigger melasma. Eating antioxidant-rich foods supports overall skin health, while managing stress helps keep hormones balanced.
Look for symmetrical brown or grayish patches on both sides of your face, particularly on your cheeks, forehead, or upper lip. The patches should be flat, smooth, and develop gradually over time. If you notice these signs, especially if you're pregnant or taking hormonal medications, see a dermatologist for proper diagnosis.
Melasma appears symmetrically on both sides of your face and is closely linked to hormonal changes. Other types of hyperpigmentation might appear randomly, result from acne scars, or develop from sun damage alone. The pattern and triggers help distinguish between different types of pigmentation.
Yes, progesterone can trigger melasma, especially when combined with estrogen. This hormonal combination stimulates melanin production in susceptible individuals. Even postmenopausal women using hormone replacement therapy can develop melasma.
Pregnancy limits treatment options since many melasma treatments aren't safe for expecting mothers. Focus on strict sun protection, gentle skincare, and vitamin C serums. Most pregnancy-related melasma fades naturally after delivery, though this can take several months.
While there's no "cure" from the inside, supporting your overall health helps. Eat antioxidant-rich foods, stay hydrated, manage stress, and ensure adequate sleep. Some people find that addressing underlying hormonal imbalances helps, but topical treatments and sun protection remain the most effective approaches.
Identifying melasma early gives you the best chance for successful treatment. Look for symmetrical patches on both sides of your face, especially if you're experiencing hormonal changes or have increased sun exposure. Remember that melasma is a manageable condition, though it requires patience and consistent care. The combination of proper diagnosis, appropriate treatment, and diligent sun protection offers the best path to clearer, more even-toned skin. If you suspect you have melasma, don't hesitate to consult with a dermatologist who can guide you toward the most effective treatment plan for your specific situation.